Best Linux distros 2024: Desktops, lightweight distros, enterprise, and cyber security
Bringing together the best Linux distros on the market today, including specialist versions for enterprise users

- Pop!_OS (Desktop)
- Arch Linux (Desktop)
- Ubuntu (Desktop)
- Debian (Desktop)
- Slackware (Desktop)
- Puppy Linux (Lightweight)
- Ubuntu MATE (Lightweight)
- Tiny Core Linux (Lightweight)
- Red Hat Enterprise Linux (Enterprise)
- Amazon Linux 2023 (Enterprise)
- Ubuntu Server (Enterprise)
- TAILS (Cyber security)
- Kali Linux (Cyber security)
- ParrotOS (Cyber security)
Our list of the best Linux distros aims to give you a sense of the sheer variety and flexibility on offer across the open source community.
There are the bigger distros on the market, the ones that have been around for years and are much-loved by fans worldwide, such as Ubuntu and Debian. There are also the smaller versions too that either serve different, sometimes niche use cases, and often build on top of the more established versions, inheriting their best bits and adding useful extras.
Linux has a fairly high barrier to entry, largely because the user interface is so different. Unlike Windows or macOS, Linux relies on its command-line tool for navigation, which can be intimidating, particularly if you have never used that function on other operating systems.
If you can get past that steep learning curve, you'll find Linux to be an incredibly satisfying operating system to use; once you sink their teeth into Linux you'll find it difficult to use anything else.
Best Linux distros 2024: Best distros for desktop
Although desktop Linux is a comparatively niche use case compared to the operating system’s ubiquitous server presence, it’s also a rewarding one. For getting things to work easily, Ubuntu-based distros can be the best choice, though distros like Arch and Slackware aren't without their charms.
Pop!_OS
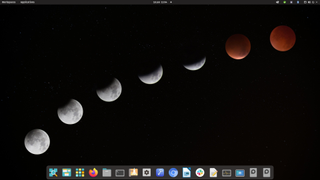
Best distro for developers and digital artists
Link: pop.system76.com/
System 76’s Pop!_OS is one of the most comfortable choices for desktop Linux users who just want to get on with things. It’s based on Ubuntu, but strips out some of the more controversial elements, such as Ubuntu’s default Snap package system, while adding useful features such as out-of-the-box support for Vulkan graphics. Its target audience is developers, digital artists, and STEM professionals.
Pop!_OS has a particularly pleasant graphical installation interface, designed to be quick and approachable. It is based on GNOME 42, and vaguely reminiscent of macOS’s GUI layout. It comes with a window manager developed in-house by System76. The firm is also an OEM and makes laptop, desktop, and server systems, all of which run the distro by default.
Arch Linux
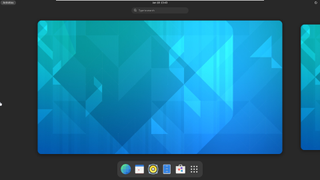
Best distro for those new to Linux
Link: archlinux.org/
Arch is a thoroughly modern, rolling-release distro that nonetheless aims to provide a classic Linux experience, giving you as much hands-on control over your OS and its configuration as possible. You’ll have to choose your own desktop environment after installation, for example.
Its official repositories typically update quickly enough, but these exist alongside the bleeding-edge community-driven AUR (Arch User Repository) system, from which you can compile packages and install them as usual via the Pacman package manager.
For those who don’t want to drive straight to the DIY ethos, Manjaro is the most popular of its derivatives, built to be more beginner-friendly, with a graphical installation interface and quality-of-life tools for driver management.
Ubuntu
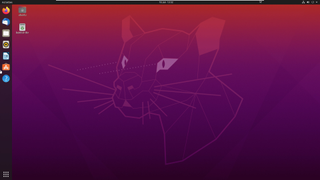
Best distro for office workstations
Link: ubuntu.com/
Based on Debian, Canonical’s Ubuntu Linux shares a significant chunk of its architecture and software, such as the friendly apt package management system.
However, it brings a lot of unique features to the table. Canonical’s Snap packages, for example, are designed to make it easy to package and distribute tamper-proof software with all necessary dependencies included, making it extremely well-suited to office workstations.
Ubuntu operates on a fast development cycle, particularly compared to Debian’s slow but stable releases. It also cheerfully provides proprietary drivers and firmware where needed.
Although Ubuntu itself is fully free, Canonical is here to make a profit, meaning that enterprise-grade support contracts are available, and the developers’ approach to security is tuned to the needs of the business.
Debian
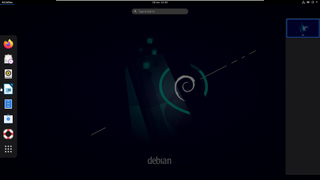
Best distro for those that prioritize stability
Link: www.debian.org/
One of the longest-established distros, dating from 1993, Debian has numerous popular derivatives, from Ubuntu to Raspberry Pi OS.
It introduced the widely-used and much-cloned apt package management system for easy software installation and removal, and to this day prioritises free, open, and non-proprietary drivers and software, as well as wide-ranging hardware support.
While Ubuntu and Red Hat are tailored to enterprise, Debian remains a firmly non-profit project dedicated to the principles of the free software movement, making it a good choice for GNU/Linux purists who want a stable OS that’s nonetheless comfortable to use, with a variety of popular GUIs to choose from.
Slackware

Best for those wanting an old-school Linux experience
Link: www.slackware.com/index.html
Another 1993-vintage distro, Slackware (no relation to the popular collaboration platform) is still very much alive and kicking, although there can be large gaps between updates. It's most recent major update, Slackware 15.0, was released in early 2022.
As you might gather from the slow release cycle, Slackware is built for long-term stability. It also maintains several classic Linux features that other distros have abandoned, making it a popular choice with many old-school users for that very reason.
It uses a BSD-style file layout and hands-on ncurses installation interface, is deliberately 'UNIX-like' and, most notably, eschews Red Hat’s now-ubiquitous systemd, so you’ll be using init rather than systemctl commands to manage services. Refreshingly, it boots to the command line by default, but you can choose from a range of desktop environments. You’ll probably also want to add a package manager such as swaret.
If you want a 'pure' and slightly old-school Linux experience, Slackware is an excellent choice and a great way of getting a handle on the underpinnings of Linux as an OS. It’ll run on almost anything, from a 486 to a Raspberry Pi, to your latest gaming PC, with support for x86, amd64, and ARM CPUs.
Best Linux distros 2024: Best lightweight distros
Not every PC is an octa-core gaming behemoth with 32GB RAM and the latest graphics card. But versatile, lightweight Linux distributions mean that an underpowered netbook or lightweight laptops for digital nomads can be brought back into use as a genuinely functional home computer, with all the security updates and modern software support that you’ll need.
Puppy Linux

Best overall lightweight Linux distro
Link: puppylinux.com/
One of the best-known lightweight Linux distros, Puppy Linux isn’t a single distribution, but rather a collection of different distros, each set up to provide a consistent user experience when it comes to look, feel, and features. Official versions are currently available based on Ubuntu, Rasbian, and Slackware, with both 32- and 64-bit versions available for most of these.
They’re all designed to be easy to use for even non-technical people, small - around 600MB or less in size - and equipped with everything you’ll need to make a PC functional. Choosing the right ‘Puppy’ can be difficult, although the project documentation is helpful in this regard.
Although 32-bit CPUs are supported, you’ll want an Athlon processor or later for more recent versions to be viable. ARM architecture is also supported in the form of Raspberry Pi.
Ubuntu MATE

Best lightweight Linux distro for newbies
Link: ubuntu-mate.org/
Ubuntu MATE - pronounced mah-tay - isn’t the lightest distro that you can acquire, as it requires at least 1GB RAM and a 64-bit Core 2 Duo equivalent processor. Despite this, it is a solid option for underpowered business notebooks or desktops, or those with an aging home office setup.
Some users find it a welcome throwback to Windows XP, and packs in all the capabilities of Ubuntu repositories. For business users switching to Linux for the first time, this could be a good choice.
Although a 32-bit x86 distribution is no longer available, you will find both 64- and 32-bit versions for Raspberry Pi, and versions specifically designed for a small range of pocket PCs.
Tiny Core Linux
Best ultra-lightweight Linux distro
Link: tinycorelinux.net/
A few versions of this ultra-lightweight distro are available to download: A fully functional command line OS image (16MB), a GUI version (21MB), and an installation image (163MB) that’ll support non-US keyboards and wireless networking, as well as giving you a range of window managers to choose from.
As you’d assume from its minuscule file size, Tiny Core doesn’t come with much software by default, but its repositories include the usual range of utilities, browsers, and office software that you’ll need to make use of your PC.
You can run it on a USB drive, CD, or stick it on a hard disk, and it’ll work on any x86 or amd64 system with at least 46 megabytes of RAM and a 486DX processor, although 128MB RAM and a P2 are recommended. Arm builds are also available, including Raspberry Pi support.
Best Linux distros 2024: The top enterprise server distros
In practice, most distros that are good on the desktop are entirely adequate for use as part of your enterprise server infrastructure, although you’ll probably want to install a version without a graphical desktop for most use cases. If you operate an enterprise server, you’ll want something with stable Long Term Support versions, responsive security updates, and that’s familiar enough to make it easy to troubleshoot. Right now, Ubuntu and Red Hat derivatives are particularly solid choices.
Red Hat Enterprise Linux

Best overall enterprise server distro
Link: www.redhat.com/en/technologies/linux-platforms/enterprise-linux
Red Hat Enterprise Linux is synonymous with big business. Although RHEL’s source code is, of course, open, it uses significant non-free, trademarked, and proprietary elements and updates that you need a subscription to access.
Red Hat emphasizes security, hands-on subscriber support, and regulatory-compliant technologies and certification. Its developers also put a lot of effort into its enterprise-grade GUI, which can be more comfortable for those who’d rather not do all their configuration at the command line.
Red Hat itself - now a subsidiary of IBM - has contributed important elements to Linux as a whole. With fully free community Red Hat derivative CentOS’s move to give up Long Term Support (LTS) versions in favor of a rolling release model (via CentOS Stream), RHEL is perhaps the best option for consistent, long-term stability for anyone who requires a Red Hat based Linux distribution for business use.
Amazon Linux 2023

Best alternative to RHEL
Link: aws.amazon.com/linux/amazon-linux-2023/
Amazon Linux 2023 is the firm’s general-purpose distro based on Red Hat package manager (RPM). It is integrated with AWS and supports widescale cloud deployment, all features of Amazon’s EC2 instances and its repositories include packages designed to seamlessly integrate with AWS’s many other services. It comes with long-term support and quarterly minor releases in addition to major releases.
Amazon Linux 2023 releases are partly based on the upstream Fedora distro. If your firm is moving machines to AWS, this could be an excellent option.
Although its VM image and containerized versions are designed first and foremost for deployment on AWS, you can download VM images for on-premises use if you want them.
Ubuntu Server

Best free enterprise server distro
Link: ubuntu.com/download/server
While most desktop Linux distros are just as capable as servers, we’re going out of our way to recommend Ubuntu for both. It’s incredibly easy to roll out a wide range of secure and fully-functional servers from its packages. It’s also free and conspicuously quick when it comes to security updates.
Its Long Term Support versions promise OS security guarantees until April 2027, though expanded security maintenance runs until April 2032.
As well as x86 architecture, it’s available for ARM, as well as IBM’s POWER server and Z mainframe platforms, although its legacy hardware support pales in comparison to Debian’s.
Ubuntu is entirely free for everyone, but enterprises can sign up for commercial support. Due to Ubuntu’s popularity, the server distro is also subject to widespread community and third-party support.
Best Linux distros 2024: Best distros for cyber security
Some firms may choose Linux because it’s free or because they don’t like being beholden to a large corporate entity. Others use Linux for security: either to maintain it or to test it. There are a number of distros designed for those who want to lock down their privacy and security at all costs, as well as distros built for infosec professionals who need to make use of more specialized tools.
TAILS

Best Linux distro for those that value privacy
Link: tails.boum.org/
If you work on other people’s computers or on public networks and you’d like to minimise the risk of your identity, communications and data being compromised, TAILS is the OS-on-a-stick for you.
Based on Debian, TAILS’ most distinctive feature is that it routes all internet traffic via TOR by default and can operate as a live distro from a USB stick. The 1.3GB image includes a GNOME 3 desktop environment, with all the conveniences of a modern desktop Linux.
Data from TAILS is never written to the hard disk, and it runs entirely using system memory which is erased when you shut it down. When it is started up again, it is always from the same clean slate, though users can configure it to retain some details in persistent storage.
Kali Linux
Best Linux distro for cyber security professionals
Link: www.kali.org/
Kali is far from an all-purpose distro, as its bread and butter is pen testing. Those looking to complete red-team security drills will find it a great environment in which to work, with great scope for the depth of development and testing that is possible within this Debian-based distro.
As mentioned, Kali Linux shines in its security applications. It contains a huge range of tools for all kinds of specific use cases, as well as both 32 and 64-bit images for different platforms.
Kali also comes with specialist hardware support, such as Kali NetHunter for Android and can even be installed on Raspberry Pi. The team has also put together detailed steps for getting Kali Linux to run on Apple hardware, though work is still ongoing to allow Linux distros to seamlessly run on M1 or M2 chips.
To complement its red-teaming distro the Kali Linux project has also released Kali Purple, a defensive distro that was released in a technical preview in March 2023. Through Kali Purple security teams can run internal wargames, and make use of more than 100 defensive tools covering encryption and decryption, security information and event management (SIEM), and more.
Kali Purple also boasts Kali Autopilot, the project’s automated attack script builder. Developers can use it to simulate attacks within their corporate environment, as well as share the scripts through an integrated hub to allow blue teams to try out threats built by the community.
ParrotOS

Best Linux distro for those that need flexibility
Link: www.parrotsec.org/
ParrotOS may be a single distro, but it comes in a range of editions to suit your company’s needs. All are based on Debian's Testing tree and they're also available with the MATE, KDE, and XFCE desktop services.
The Home Edition (shown above) is a lightweight OS for daily use. It is especially suited for privacy purposes, with Parrot stating that it also makes a good environment for software development and daily business use.
To complement the latter, Parrot comes with the LibreOffice suite pre-installed as well as a repository of popular creative tools such as OBS, Blender, and Krita. Also included is a range of encryption tools like zulucrypt as well as anonsurf, a tool that routes your internet packets through TOR relay to hide your IP address.
For the more security-minded user, ParrotOS Security Edition could be best. Intended as an alternative to Kali Linux, it comes packed with over 600 tools for Blue and red teams including those for network analysis, Wi-Fi penetration, reverse engineering, and more.
Full disk encryption keeps sensitive data safe, and the distro is entirely free of telemetry software to ensure user activity is not tracked. Security Edition is also available for cloud environments, virtual machines, and other special use cases through ParrotOS Cloud Edition.
ParrotOS Hack The Box Edition, which is intended for those without the wherewithal to set up a custom hacking VM, could prove perfect for smaller firms. This is accessible through a web browser, and lightweight enough that any team could use it without needing extra resources.
What is a Linux distro?
A Linux distribution, or 'distro', is a custom version of the core Linux kernel that has typically been designed with a specific purpose or function in mind. These modified versions offer bespoke toolsets and experiences that differ to that of the standard Linux OS.
As Linux is an open source operating system, its development is handled by its community. Any user is able to take the core Linux kernel and modify it to produce their own custom OS, and distribute this freely to the community. This usually involves stripping out unnecessary features, adding new tools, or changing the look or feel, such as the addition of a GUI.
Our list of the best Linux distros is overwhelmingly made up of those versions that are designed for specific purposes in mind, such as offering specialist cyber security tools or support for enterprise servers. Each entry has taken the core Linux kernel, a handful of GNU packages, and a bunch of software components to craft something unique.
This means that once you understand the fundamentals of using GNU/Linux, you can apply that knowledge to any other Linux OS and be confident that everything will work more or less as you expect.
While all Linux distros rely to some extent on voluntary contributions from a community of developers for their continued development and stability, some distros are backed by large commercial software development organizations, with Canonical (which develops Ubuntu) and Red Hat (RHEL) being key examples. Because they benefit from full-time corporate support and upkeep, these distros are often updated more frequently than at least some of their community rivals and may be better options for businesses that prioritize stability.
Get the ITPro. daily newsletter
Receive our latest news, industry updates, featured resources and more. Sign up today to receive our FREE report on AI cyber crime & security - newly updated for 2024.
K.G. is a journalist, technical writer, developer and software preservationist. Alongside the accumulated experience of over 20 years spent working with Linux and other free/libre/open source software, their areas of special interest include IT security, anti-malware and antivirus, VPNs, identity and password management, SaaS infrastructure and its alternatives.
You can get in touch with K.G. via email at reviews@kgorphanides.com.






